Jaw pain

Jaw pain can range from mild to unbearable. It can be caused by dental issues or more serious conditions. Trying to figure out the exact cause of jaw pain on your own can be difficult, because it is not always a dental problem. Therefore, regardless of the underlying cause, it is important to pay attention to jaw pain.
Why does the jaw hurt? What are the accompanying symptoms of jaw pain? How is it treated? How can it be associated with a heart attack?
Common Causes
Jaw pain is most commonly caused by the following general reasons:
Temporomandibular Joint (TMJ) Disorder
The TMJ is one of the most complex joints in the body, connecting the lower jaw to the skull. It is responsible for the movement of the lower jaw in different directions.
Temporomandibular Joint Disorder (TMJD) refers to any pathology that disrupts temporomandibular joint function. In addition to pain, the joint may experience clicking during chewing or opening of the mouth. In some cases, TMJD can cause the jaw to become stuck in an open or closed position.
Common causes of TMJD development include:
Malocclusion (abnormal bite)
Errors in orthodontic treatment
Dental restoration (filling/crown) that misaligns the bite due to improper positioning in the dental arch
Bruxism (teeth grinding) and increased tooth wear
Early loss of molar teeth.
Teeth Grinding (Bruxism)
Uncontrolled teeth grinding is the most common cause of jaw pain. Bruxism develops due to structural and functional abnormalities of the dental system or psycho emotional problems.
As a result of frequent spasms in the chewing muscles, the temporomandibular system becomes overloaded. This leads to pain in the area of the TMJ. The pain may be felt in the ear when yawning. Additionally, over time, the condition of the teeth significantly deteriorates. Chips and cracks gradually form on the teeth. Enamel wears down, and hypersensitivity develops. Teeth may become loose.
Dental diseases
Jaw pain can arise from dental conditions such as deep cavities, pulpitis, and others. These diseases do not directly affect the jaw, but the pain they cause can radiate to the jaw. If an infection penetrates the tooth root, a throbbing pain can spread through the nerve endings. Jaw pain occurs in the area of the affected tooth, and the discomfort may intensify at night.
Sialadenitis
Large salivary glands are located on both sides of the lower jaw, along with numerous small ducts that deliver saliva into the oral cavity. Infectious involvement of these glands can lead to a slowdown or blockage of saliva flow. Over time, pathogens develop in stagnant saliva, resulting in sialadenitis. The condition is accompanied by soft tissue swelling and the formation of a painful lump in the cheek or under the chin.
Sinus Problems
The sinuses (paranasal sinuses) are paired cavities within the skull bones, connected to the nasal cavity. When bacteria enter the sinuses, excessive mucus production occurs. This excess mucus can exert pressure on the jaw joint and trigger pain.
Trauma
A painful jaw can result from a fracture or dislocation. Mechanical damage can be identified if there have been falls or blows to the face. Trauma can also occur after dental treatment, such as a complex tooth extraction. Dislocation of the jaw can happen with excessive mouth opening.
Rare Causes
Jaw pain is typically associated with TMJ disorders, tissue infections in the mouth, or dental problems. However, there are other, less known reasons for jaw pain.
Heart Attack
The main symptoms of a heart attack include pain and discomfort in the center or left side of the chest. However, other symptoms are also possible, such as difficulty breathing, nausea, dizziness, as well as pain in the lower jaw, back, arms, and other areas.
Autoimmune Conditions
Conditions like lupus, rheumatoid arthritis, rheumatic polymyalgia, and other autoimmune disorders are associated with joint pain, including the jaw. The pain often resembles symptoms of TMJ disorders.
Trigeminal neuralgia
When the facial nerves are affected, sharp shooting pain occurs in the lower jaw. It feels like electric shocks that become more painful with slight facial muscle movements. Patients may have difficulty chewing, speaking, blowing their nose, or laughing. The pain can be felt in the chest, eyes, and forehead. Partial paralysis and pronounced facial asymmetry are possible symptoms as well.
Osteonecrosis of the Jaw
Osteonecrosis occurs when there is a disruption in blood supply to the bone tissues, leading to bone death. This condition causes severe pain, prominently in the jaw. It develops due to significant bone trauma, smoking, alcohol abuse, poor blood clotting, radiation therapy, and other factors.
Cancer
Malignant tumors in the oral cavity can also cause jaw pain. They can affect the lips, oral tissues, the back of the throat, and other areas. Chewing function and jaw movement may be impaired. Jaw pain caused by cancer is typically dull in nature.
Symptoms
Jaw pain can be accompanied by the following symptoms:
Facial tenderness
Dull pain in the ear
Clicking sounds during jaw movement while talking or chewing
Limited range of jaw motion (inability to fully open the mouth)
Jaw getting stuck in an open or closed position
Headaches in the temples and around the eyes
Tinnitus (ringing in the ears)
Neck and shoulder pain
Sinus pain
Dizziness
Back pain
Jaw pain and headaches
Headaches are the most common symptoms of TMJ dysfunction. TMJ-related pain is often mistaken for migraines. Some mistakenly believe that severe headaches are due to genetic factors or excessive tension and stress. However, research confirms the interconnection between temporomandibular joint abnormalities and headaches.
The jaw joint and head are closely linked through muscular structures. Normally, when the TMJ is not involved, the muscles are relaxed. However, chronic emotional stress, a disrupted bite, or abnormal tooth positioning can lead to an overload of the jaw muscles. Over time, headaches and TMJ dysfunction develop.
Another cause for headaches is bruxism. Uncontrolled spasms of the chewing muscles can trigger muscle pain that is felt in the head. Patients complain that even rest does not alleviate the discomfort, and pain-relieving medications only provide temporary relief.

This patient came to the clinic complaining of headaches and pain while chewing. She was also concerned about problems with the aesthetics of her face, especially regarding the complete collapse of the front part of her face due to an incorrect bite.
Treatment:Dr. TETRI and Dr. KOVAL performed the treatment. In the first stage, Dr. KOVAL conducted orthodontic treatment. Then, Dr. TETRI performed a full mouth reconstruction using the principles of gneuromuscular dentistry and the unique Digital Smile Design technology, which allowed for the patient to visualize her smile before treatment even began. During treatment, the bite was raised, cosmetic gum surgery was performed, and veneers were placed.
The result:After 7 months, the final results were visible. The profile of the face was radically changed, its correct proportions were restored, and the smile appeared natural, brighter, and 10-15 years younger.
Jaw pain on one side under ear
Jaw and ear pain on one side can also be associated with TMJ dysfunction. The ear is a paired organ that is filled with nerve endings and blood vessels. If the movements of the joint are asymmetrical, it creates tension in the joint capsule. The pain is then felt in the ear. The patient may not experience discomfort while chewing, as the other side of the jaw compensates for the load. However, the joint starts to react to this, resulting in pain below the ear, either on the left or right side of the jawbone.
When should I see a TMJ doctor?
It is recommended to seek immediate medical attention if you experience:
Persistent and severe jaw pain
Chronic headaches or earaches
Clicking or popping sounds
Restricted jaw movement
Pain after unsuccessful self-treatment
What to do before visiting the doctor
When experiencing jaw pain, the process of chewing can exacerbate the discomfort. It is important to pay careful attention to what you eat. We recommend cutting food into small pieces and consuming soft products such as:
Fruits and vegetables: bananas, pears, melon, applesauce, smoothies, fruit yogurts. For vegetables, try cooked carrots, zucchini, and peas.
Eggs, legumes, chicken, and fish.
Mashed potatoes, oatmeal, and other porridges.
Dairy products: cheese, cottage cheese, kefir, yogurts, and others.
This diet ensures safe food consumption while providing the necessary micronutrients for the body.
Diagnosing Jaw Pain
The diagnosis of temporomandibular joint disorders involves a comprehensive examination of the patient. It is conducted by a gnathologist, a specialist who identifies and treats disorders of the dental and jaw systems affecting chewing function. During the diagnostic stage, the gnathologist needs to differentiate TMJ disorders from dislocations, injuries, and other pathological conditions.
Key stages of diagnosis include:
Gathering a complete medical history: The gnathologist inquires about the patient’s complaints, listens to sounds of the TMJ during jaw movement, and notes any deviations during bite closure.
Computer tomography.
TMJ magnetic resonance imaging (if necessary).
Creating diagnostic casts.
Evaluation of the functionality of the chewing muscles, bite quality, and range of motion of the lower jaw.
Creating intraoral/extraoral photographic records.
Based on the diagnostic results, the doctor develops potential treatment plans and offers therapy options to the patient. If necessary, the gnathologist may involve other specialists during the diagnostic stage.
Treatment Jaw Pain
The treatment protocol depends on the specific clinical case, but the main treatment scheme includes the following stages:
Pain and Muscle Tension Relief
Splint Therapy
It involves restoring TMJ functions using occlusal splints. A splint is a relief cap made of dense plastic that fits over the teeth. The splint’s relief ensures the correct trajectory of the lower jaw during bite closure, restores the physiological position of the jaw joint, normalizes the tone of the chewing muscles, and stretches the joint ligaments. The patient wears the splint around the clock and only removes it for daily care. They can consume food without removing the splint from their mouth.
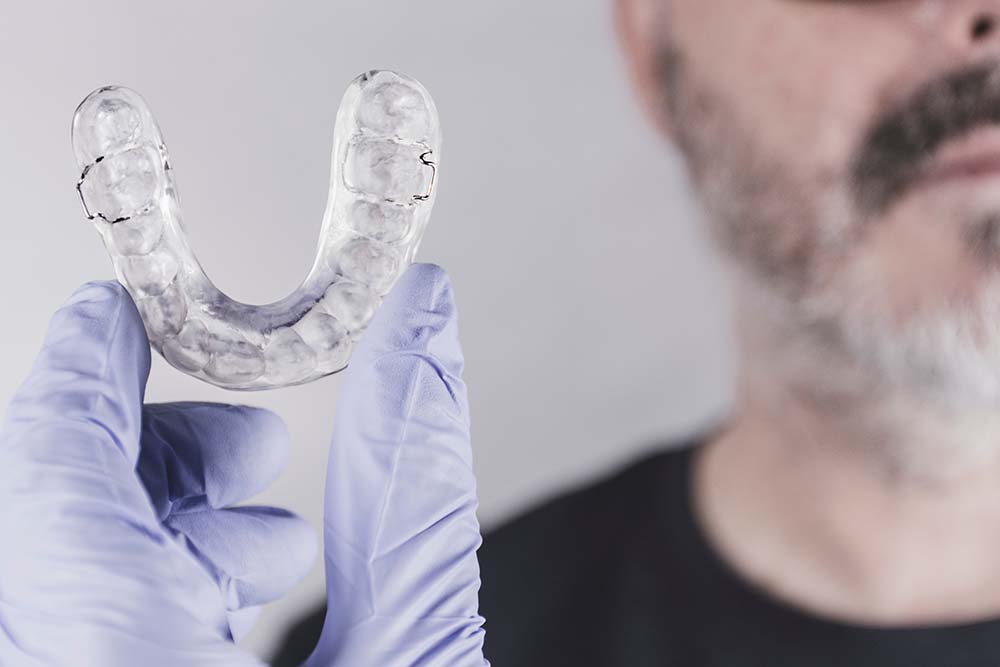
Occlusal splints are custom-made based on the patient’s individual parameters determined during the diagnostic process. The duration of wearing the splint ranges from 2 to 6 months, depending on the extent of TMJ dysfunction.
Splint therapy gently restores the condition and functions of the TMJ without surgery. It alleviates headaches, neck pain, clicking and popping sounds during jaw movement, relieves tension from the joint muscles, and tightens facial skin.
TENS Therapy
Transcutaneous Electrical Nerve Stimulation (TENS) involves low-frequency stimulation of facial muscles and nerve endings using microcurrents. At Tetris’ Smile clinic, J5 Dental TENS apparatus is used for treatment. This device includes sensors that are placed on the face and neck. The range of wave frequencies, from 0.5 to 50 Hz, is completely safe for health.
The device analyzes the condition of the facial muscles and detects areas of muscle tension. During the procedure, microcurrents are applied to these problem areas, stimulating muscle fibers. This improves tissue nutrition and blood circulation in the capillaries, relaxes muscles, eliminates spasms, and restores the correct position of the TMJ and lower jaw.
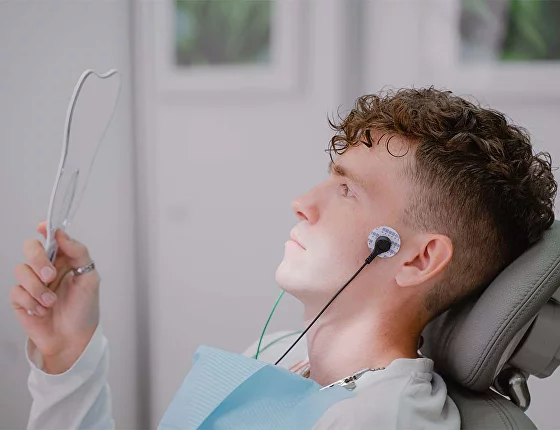
TENS therapy smoothes facial wrinkles, reduces the intensity of headaches, and restores mobility in the neck. It eliminates jaw pain and discomfort.
Injections of neuroproteins
Injections of neuroproteins are used to effectively treat bruxism and muscle hypertonicity. These injections block nerve impulses and relieve tension from the facial muscles. The effect of the injection is immediate, releasing muscle tension and completely relaxing the jaw muscles. The lower jaw and the jaw joint return to their natural physiological position.
The neuroproteins are injected into specific points and do not affect the functionality of other facial muscles. The effects of a single procedure last for several months. After botulinum toxin therapy, it becomes easier for the patient to eliminate harmful habits such as jaw clenching and teeth grinding.
After completing this stage, the doctor may prescribe medication for the patient.
Restoration of Missing Teeth
The integrity of the dental arch can be restored using fixed dental prostheses on natural teeth or implants. Dentists recommend choosing dental implantation, which permanently resolves dental issues. Implant-supported prostheses fully restore the aesthetics and functionality of the missing tooth, evenly distribute the load on the bone, and prevent bone loss. This type of construction does not require preparation of neighboring healthy teeth.
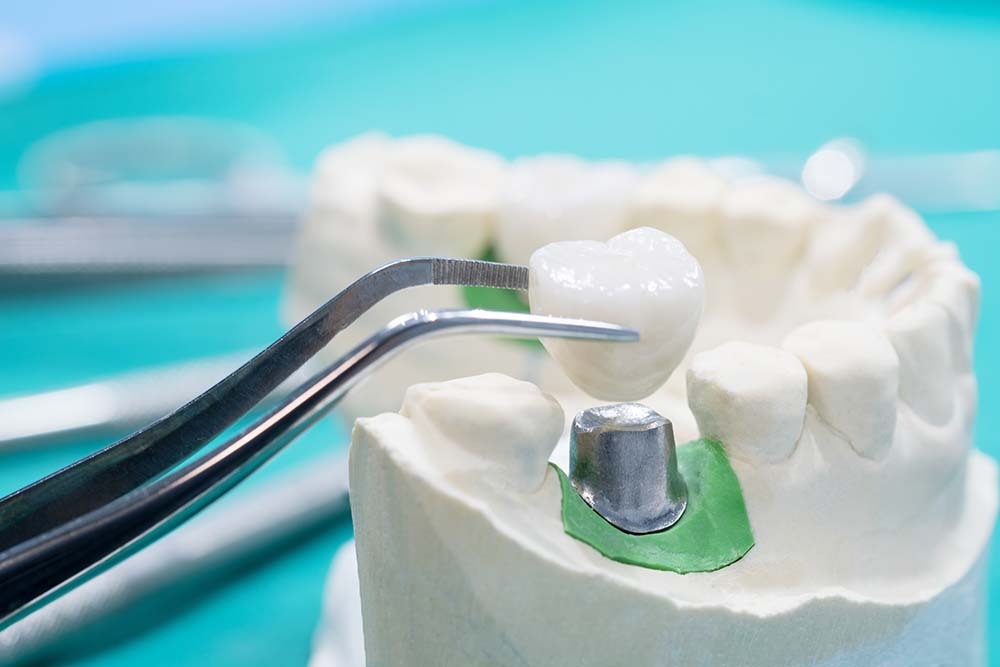
Prevention
These measures can help prevent or mitigate the progression of TMJ disorders:
Manage stress levels
Avoid excessive strain on the jaw joint
Exclude hard foods from the diet
Minimize caffeine consumption (as it can contribute to muscle tension)
Undergo orthodontic treatment if needed
Treat bruxism if you experience any of its symptoms


